Here we are going to share information on the topic “Measles symptoms in adults.” Welcome to our discussion on measles symptoms in adults. Measles symptoms in adults can often be overlooked or mistaken for other illnesses, yet it’s crucial to recognize the distinct signs associated with this contagious virus. Measles symptoms in adults encompass a range of manifestations, from the classic rash and fever to more severe complications.
Understanding the nuances of measles symptoms in adults is vital for early detection and appropriate management. Throughout this exploration of measles symptoms in adults, we’ll delve into the distinct manifestations that characterize this infectious disease and underscore the importance of awareness and preventive measures. So, let’s delve deeper into the topic of measles symptoms in adults to gain a comprehensive understanding of this significant health concern.
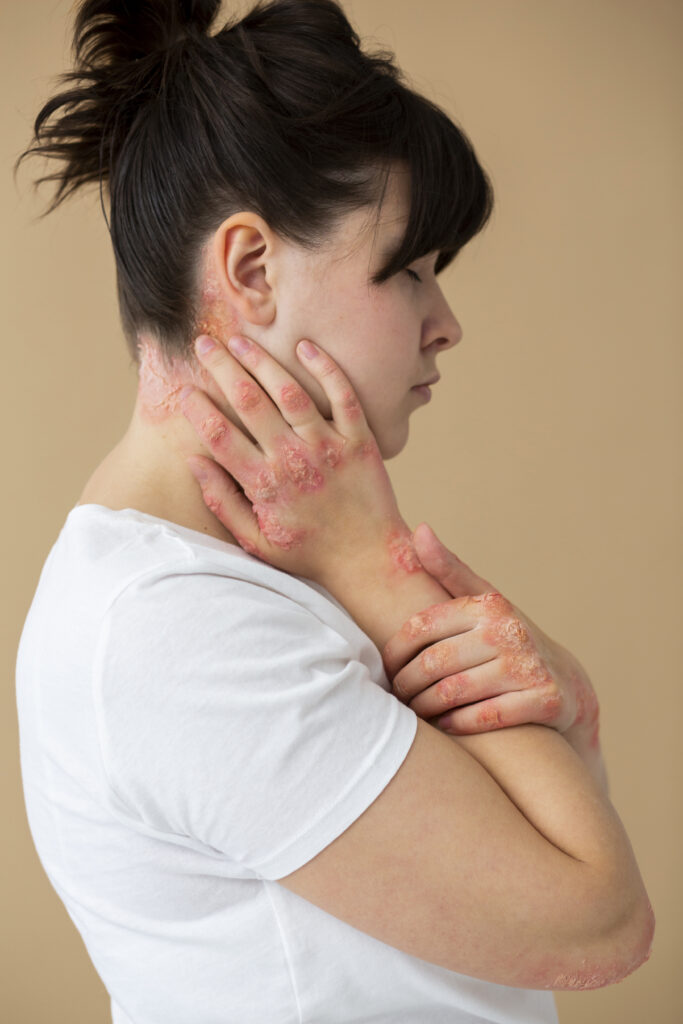
Measles symptoms in adults
What is measles?
Measles is a highly transmissible virus. Its distinctive red, blotchy rash is what makes it most famous. Measles can be extremely dangerous, resulting in hospital stays and even fatalities.
Before the measles vaccination was introduced to the pediatric immunization schedule in the middle of the 1970s, the disease was widespread in Australia. Australia was proclaimed measles-free in 2014. Even now, outbreaks occasionally happen when tourists who contract the disease abroad return to Australia contaminated.
The advice on this page is geared toward adults and kids who are older than five. To find out more, go to the Pregnancy, Birth, and Baby website.
What measles symptoms are present?
Measles symptoms typically start to show up ten days after contact with an infected person.
Although a blotchy red rash is the most well-known measles sign, it is not always the first to appear.
The typical course of measles is a flu-like disease that lasts two to four days and has the following symptoms:
- Fever
- tiredness
- severe conjunctivitis from coughing (red eyes)
- White patches in the mouth and runny nose (known as Koplik spots)
The rash develops between days three and seven of the sickness. Usually, it’s not irritating; it’s just blotchy and red. Usually, a measles rash begins on the head and progresses to the rest of the body. Usually, it lasts four to seven days.
The infection progresses over a period of two to three weeks.
Both incubation and infection.
The first 10 to 14 days following infection are when the measles virus multiplies within the body. During this period, there are no measles signs or symptoms.
Symptoms and indicators that are vague.
A low to moderate fever, along with other symptoms such as a runny nose, sore throat, swollen eyes, and conjunctivitis, are the usual first signs of measles. The duration of this comparatively mild illness is two to three days.
Acute disease with rash.
Little red dots, some of which are slightly elevated, make up the rash. The skin appears splotchy red due to spots and pimples in tightly clustered formations. First, the face gets red.
The rash appears on the arms, chest, and back over the course of the following few days, before moving on to the thighs, lower legs, and feet. Simultaneously, the fever spikes, frequently reaching temperatures between 104 and 105.8 F. (40 to 41 C).
Recovery.
One may experience a seven-day rash from measles. The face rash eventually goes away, followed by the thighs and feet. The cough and skin darkening or peeling where the rash was may persist for around 10 days after other symptoms of the sickness go away.
Why does measles occur?
A virus is the cause of measles.
How is the disease spreading?
Coming into contact with an infected person can spread the measles. This could originate from:
interpersonal contact sneeze and coughing
For up to two hours, measles virus particles can remain in a room and spread to other people. The virus may be on surfaces or in the air.
The measles spreads easily. Typically, the day before you start feeling sick to four days after your rash emerges is when you are most contagious.
Nine out of ten individuals who are susceptible to the measles will contract it from an infected person. In order to protect yourself from the measles, you must:
- Held a measles vaccination
- Having previously contracted the measles
Who is susceptible to the measles?
- If they are not immune, anyone can contract the measles at any age.
- Individuals with compromised immune systems are susceptible to:
- become infected with measles and experience severe complications
- Pregnancy and measles
See your doctor for a pre-conception physical if you intend to become pregnant. Typically, this entails confirming your immunity to diseases like the measles.
The risk of miscarriage or premature labor increases if you contract the measles while pregnant.
It is not recommended to receive measles immunizations when pregnant.
When should I visit my physician?
You should contact your doctor right immediately if you suspect you may have the measles. If you have come into contact with someone who has the measles, you should also consult your physician.
Since you don’t want to spread infection to others in the waiting area, avoid going to the clinic. Instead, give your doctor a call, and they will advise you on the best time to visit them. Inquire with your physician about the availability of a telemedicine appointment or house visit.
Measles can be an extremely serious illness, requiring hospitalization for certain patients.
Additionally, your doctor will provide you advice on how to keep other members of your home safe.
It’s crucial to stay at home if you suspect you have the measles in order to prevent the infection from spreading. When you’re cleared to resume work or school, your doctor will let you know.
It is required to report measles cases. This implies that the medical professional who makes the measles diagnosis must notify the local health authority of the case. They’ll take action to stop or manage an outbreak. Because measles is highly contagious, contact tracing is typically required. In order to find out who has recently been in close contact with you, contact tracers will speak with you.
If complications arise from the illness, other symptoms might appear. Consult your physician if you suspect you may have measles and if your symptoms worsen or develop new ones.
How is a measles diagnosis made?
By asking you about your symptoms and seeing your rash, your doctor can make the diagnosis of measles. They might additionally inquire:
If you’ve had contact with a measles patient, please provide the details of your immunization history.
Your physician might recommend blood testing if they believe you have the measles. The diagnosis can be verified by the test findings.
How does one cure measles?
There isn’t a specific medication or therapy for measles.
You can attempt the following at home to try to reduce your symptoms:
- obtain enough sleep
- consume a lot of liquids
- To treat any feverish symptoms, take paracetamol; carefully follow the directions on the package.
- Since a virus, not bacteria, causes measles, antibiotics will not aid in your recovery.
In the event that your symptoms worsen or you encounter complications, you might require medical treatment.
What occurs if I come into contact with a measles victim?
You will be offered treatment if you are not immune to the measles and have had close contact with an infectious person. This lowers the likelihood of becoming ill and is referred to as post-exposure prophylaxis.
The standard measles post-exposure prophylaxis involves immunization. If vaccinations are not an option for you, you might receive medication that contains measles-preventing antibodies. These must be administered within 72 hours of exposure in order to be effective.
How can the measles be avoided?
It is best to be vaccinated against measles.
As part of a combination immunization, the measles vaccine is administered for:
- rubella-mumps-measles (known as MMR)
- Mumps, rubella, varicella, and measles (known as MMR-V)
- Both have comparable adverse effects and are incredibly effective. Which vaccination is best for you can be determined by your doctor.
- In Australia, 99 percent of people may avoid contracting the virus after receiving two measles vaccinations.
Measles vaccination is highly advised for those who are not immune:
who travel while working in the healthcare industry, in childcare, or in aged care
Vaccination against measles shouldn’t be administered to:
- individuals with compromised immune systems who are pregnant
- After the immunization, you should wait 28 days before getting pregnant. Therefore, following your second immunization, you should utilize contraception for at least a month.
Implications from contracting the measles
Complications from the measles are more prevalent in those who are:
impaired immune system (where the immune system is not working as well as it should)
inadequately fed
Possible complications include:
- medial otitis (ear infection)
- pneumonia (lung infection)
- encephalitis (inflammation of the brain)
- meningitis (inflammation of the lining of the brain)
Ten percent of measles patients experience problems. Problems might have long-term consequences or even result in death.
Conclusion
Measles symptoms in adults
In conclusion, prompt diagnosis and effective medical management depend on an awareness of adult measles symptoms. Even though measles is typically associated with children, adults can contract the virus and experience mild to severe symptoms.
Identifying symptoms like fever, rash, cough, and sore throat can help with timely treatment and help avoid complications. Furthermore, immunization continues to be the most effective way to prevent measles, underscoring the significance of immunization campaigns and preserving herd immunity to shield people of all ages from this extremely dangerous illness.

Frequently asked questions
Measles symptoms in adults
What are the first symptoms of measles in adults?
After being infected, measles usually manifests its initial symptoms 10 days later. These may include symptoms of a cold, such as coughing, sneezing, and a runny nose. inflamed, painful eyes that could be light-sensitive.
How do you treat measles in adults?
Once contracted, there is no particular therapy for measles. Treatment entails treating or avoiding problems in addition to offering comfort measures to ease symptoms, such as rest.
How do you check for measles?
For both outbreaks and sporadic measles cases, laboratory confirmation is necessary. The most popular techniques for verifying measles infection are the detection of measles-specific IgM antibodies in serum and measles RNA by real-time polymerase chain reaction (RT-PCR) in respiratory samples.
What are the danger signs of measles?
After coming into contact with the virus, measles symptoms usually manifest 7 to 14 days later and include fever, coughing, a runny nose, and watery eyes. 3 to 5 days after the onset of symptoms, the measles rash emerges.
How long does measles last in adults?
It gradually spreads to the hands and feet over the course of three days. It often fades after 5–7 days. The majority of measles deaths are caused by the disease’s complications.
Can I take a bath if I have measles?
The goal of measles treatment is to reduce discomfort as the illness progresses. Since measles patients frequently have high fevers, taking a mild bath might lower the body temperature and ease pain and other symptoms. You might try adding oatmeal or mineral salts to the bath water to help soothe itchy skin.
So, this is how the topic “Measles symptoms in adults” has been addressed.
For more information related to these topics,
You may also visit our Instagram page by
Thank you !